Say Goodbye to Discomfort!
Expert Care Tailored to You
Innovative Services & Techniques
Be Part of a Success Story
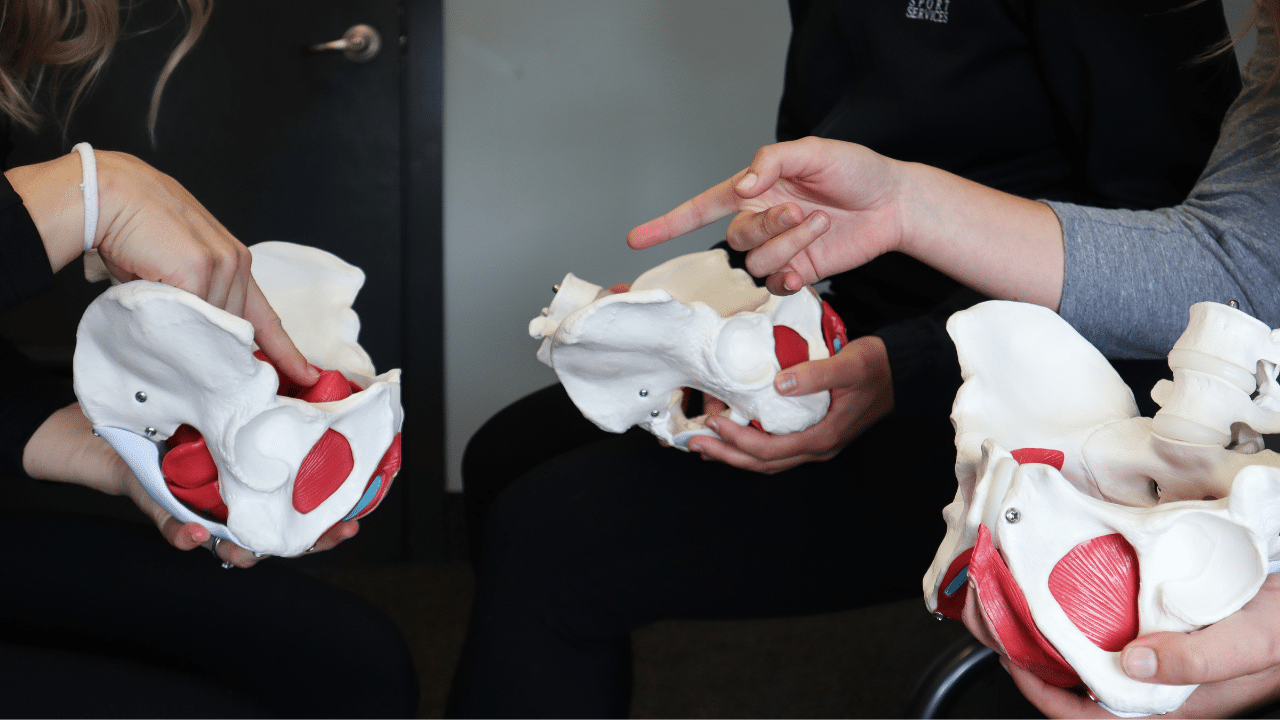
Pelvic floor physiotherapy includes the assessment and treatment of various conditions that involve pelvic floor dysfunction, or symptoms that manifest in this area.
It can be a crucial part of an individual’s complete medical care. The pelvic floor includes muscles, ligaments, nerves and connective tissue. It plays an important role in the body by providing support for the bladder, genitals, uterus and anus. Pelvic floor pain or dysfunction can impact all genders, ages, and stages of life.
Concerns of the pelvic floor are widespread and diverse. Get started on your journey to more comfort, function, and freedom by identifying the symptom(s) you’re experiencing from our list below! Hover over each card for more information on the ways this theme can impact pelvic health.
Not seeing your unique circumstance captured on these cards?
Contact our team to find out if pelvic floor therapy is right for you!

BLADDER
BLADDER-RELATED CONCERNS MAY INCLUDE:
- Prostate pain or enlargement
- Stress, urge, and mixed incontinence
- Overactive bladder
- Interstitial cystitis

CORE & STRENGTH
CORE & STRENGTH-RELATED CONCERNS MAY INCLUDE:
- Athletic Pubalgia
- Sports hernia
- Athletic-based incontinence
- Hip, low-back, SIJ, or groin pain with athletics

SEX
SEX-RELATED CONCERNS MAY INCLUDE:
- Pain with sex (vaginal, rectal, orthopaedic)
- Leakage with sex
- Weak pelvic muscles/poor sensation

PAIN
(WITHIN THE PELVIS)
PAIN-RELATED CONCERNS MAY INCLUDE:
- Post-radiation pain
- Prostate pain
- Vaginismus
- Vulvodynia
- Menstrual pain
- Undiagnosed pelvic pain

PROLAPSE
PROLAPSE-RELATED CONCERNS MAY INCLUDE:
- Vaginal vault prolapse
- Uterine prolapse
- Cystocele
- Rectocele
- Enterocele

Pain
(outside the pelvis)
PAIN-RELATED CONCERNS MAY INCLUDE
- Hip pain
- Coccyx/tailbone pain
- Pubic symph pain
- Low-back pain

PREGNANCY
PREGNANCY-RELATED CONCERNS MAY INCLUDE:
- Preparation for labour/delivery
- Pelvic pain (low back, SIJ, PSD, coccyx)
- Core strength (diastasis recti)
- Postpartum care and return to activity

BOWEL
BOWEL-RELATED CONCERNS MAY INCLUDE:
- Constipation
- Bowel incontinence (gas or stool)
- Bowel pain, poor motility
- Urgency

POST-OPERATIVE
POST-OPERATIVE-RELATED CONCERNS MAY INCLUDE
- Abdominal surgery (appendectomy, bowel, gallbladder, hernia, diastasis repair, abdominoplasty)
- Gynecologic surgery
- Prostate surgery
- Pelvic cancer care
Your pelvic health therapist!
Craven SPORT Services is the proud home of an excellent pelvic health physiotherapist, Hayley Braun. With an unwavering commitment to our clients’ well-being, Hayley is dedicated to delivering a level of compassion and care that every individual deserves.
Contact our team to schedule a session with Hayley and get started on your journey!
What to expect during pelvic floor therapy
The treatments involved in pelvic floor therapy are as diverse as the many symptoms or situations that may
prompt a first appointment! Yet with that in mind, here is a general structure of what you can expect during
your pelvic health journey:
Assessment
- Before pelvic floor treatment begins, your pelvic health physiotherapist will take your full medical history and thoroughly discuss your current concerns, symptoms, and goals.
- With informed consent, your pelvic floor physiotherapist will perform a physical assessment of the joints and tissues affecting the area. This may include both internal and external examinations to identify the affected tissues that may be contributing to your urinary, bowel, pelvic, or abdominal symptoms. Informed consent is a huge part of pelvic health: you will always have the option to discuss or refrain from certain types of assessment if you are not comfortable doing so.
- Common areas that refer pain to the pelvic region include: the abdomen, lower back, hips, pubic symphysis (the front part of your pubic bones) and sacro-iliac joint (the joint formed by the sacrum and ilium from your low back to your coccyx). You pelvic health therapist may assess if/how these regions are contributing to your symptoms.
- Based on your examination, your pelvic health physiotherapist will work with you to put together a plan of care that is specific to your particular goals, symptoms and dysfunction. Since every person has a unique case, it is important that your treatment is customized to address your specific needs
Treatment
There are various modes of pelvic floor treatment that are well-supported by the scientific literature and can be effectively incorporated as part of your care. Some of these treatment options include:
EDUCATION
Education is power! You cannot under-estimate the importance of knowledge. Understanding the anatomy and physiology of the pelvic floor, posture education as well as knowing how to deal with chronic pain symptoms are vital to your recovery. Many clients have improved their symptoms by simply understanding how various aspects such as lifestyle, diet, urinary and bowel hygiene can affect the pelvic floor.
PERSONALIZED EXERCISE PROGRAM
As with other musculo-skeletal joints in the body, an individualized exercise program including stretching, strengthening, proper posture and breathing techniques are essential for overall pelvic health. Areas within the pelvic floor and other muscles surrounding the pelvis, thorax and lower limbs will be targeted.
BLADDER TRAINING
It is important to review your voiding patterns with your therapist to ensure appropriate bladder and bowel habits. This is essential in helping to normalize your overall pelvic function.
MANUAL THERAPY
This is presently the preferred method when treating pelvic floor dysfunction. It involves various hands-on techniques such as: stretching, facilitation, soft tissue massage, mobilization as well as connective tissue, myofascial and trigger point release techniques to the affected muscles and tissue.
OTHER TREATMENTS TO MINIMIZE PAIN
This may include the use of heat, cold, trans-cutaneous electrical nerve stimulation (TENS), interferential current (IFC), guided imagery, breathing and relaxation techniques. Your therapist will be happy to discuss these and other options with you.

Insurance Coverage
- We accept numerous insurance types and providers, including those within the Telus Health network and Sunlife. A complete list of insurance companies we are able to directly bill can be found here.
- Direct billing is available through the Telus Health network and Sunlife.
- Please note, we are only able to directly bill to the primary insurance plan. Clients will have to submit to any secondary insurance plans.
- Extended health benefits may partially or fully cover your treatment.
- Your treatment may be partially or fully covered if you were injured in a motor vehicle collision.
- We work with WCB claims.
Areas We Serve
- Saskatoon
- City Park
- North Park
- River Heights
- Broadway
- Stonebridge
- Kensington
- Montgomery
- Martensville
- Downtown
- Nutana
- Sutherland
- Mayfair
- Riversdale
- University Heights
- Evergreen
- Rosewood
- Warman
- Lawson Heights
- Caswell Hill
- Greystone Heights
- Lakeridge
- Silverspring
- Aspen Ridge
- Willowgrove
- And More!
Explore Our Health & Wellness Blog Posts

Neck Pain Solutions: How Physiotherapy Can Improve Your Condition
Dealing with neck pain can be a debilitating experience, affecting your daily activities and overall quality of life. This blog post explores the role of

Optimizing the Timing of Physiotherapy Exercises for Enhanced Recovery
When starting a physiotherapy regimen, the timing of your exercises can play a pivotal role in determining the effectiveness of your recovery and overall physical

Are You Experiencing Stress-Related Headaches? PT Can Help!
Dealing with headaches on a daily basis can be extremely isolating and exhausting. Did you know headaches are the third most common type of pain?

Nutritional Changes Can Help You Get Rid of Pain and Inflammation
If you already see a physiotherapist for internal inflammation, you are aware that this is a serious issue that can have a negative impact on

Don’t Ignore Your Back Pain; Seek Physiotherapy Assistance
The majority of people will suffer from back pain at some point in their lives. This is not to say that you should accept your
Physiotherapy Could Help You Avoid Surgery Altogether!
Are you frustrated by your recurring pain? Do you feel as if you’re out of options and are now contemplating surgery? At Craven Sport Services
Pelvic Floor Physiotherapy Saskatoon FAQs
CANCELLATION POLICY: CRAVEN SPORT SERVICES RESERVES THE RIGHT TO CHARGE A CANCELLATION FEE OF $50.00 FOR ONE HOUR MISSED APPOINTMENTS AND $25.00 FOR HALF HOUR MISSED APPOINTMENTS, OR WHEN LESS THAN 24 HOURS CANCELLATION NOTICE IS PROVIDED PRIOR TO A CLIENT’S SCHEDULED APPOINTMENT TIME. AFTER TWO OR MORE LATE CANCELLATIONS/NO SHOWS, THE CLIENT WILL BE REQUIRED TO PAY FOR THE FULL AMOUNT OF THE APPOINTMENT.
CRAVEN SPORT SERVICES MAIN CLINIC
HOURS OF OPERATION:
- Mondays: 7:00am – 7:00pm
- Tuesdays: 7:00am – 7:00pm
- Wednesdays: 7:00am – 7:00pm
- Thursdays: 7:00am – 7:00pm
- Fridays: 7:00am – 6:00pm
- Saturdays: Closed
- Sundays: Closed
CRAVEN SPORT SERVICES TRAINING CENTER
HOURS OF OPERATION:
- Mondays: 6:00am – 9:00pm
- Tuesdays: 7:00am – 9:00pm
- Wednesdays: 6:00am – 9:00pm
- Thursdays: 7:00am – 9:00pm
- Fridays: 6:00am – 7:00pm
- Saturdays: 7:30am – 1:30pm
- Sundays: Closed
CRAVEN SPORT SERVICES MARTENSVILLE LOCATION
- Martensville Rec Centre, Williams Family Fieldhouse - 2nd floor
- 100 Main Street West, Martensville, SK S0K 2T0
- Located on the west side of Hwy 12 overpass off of Mierau Rd
- PH: 306-934-2011
- EMAIL: CSS@CRAVENSPORTSERVICES.CA
HOURS OF OPERATION:
- Mondays: 7:00am - 5:00pm
- Tuesdays: 7:00am - 5:00pm
- Wednesdays: 7:00am - 5:00pm
- Thursdays: 7:00am - 5:00pm
- Fridays: By Appointment
- Saturdays: By Appointment
- Sundays: By Appointment